This web page was produced as an assignment for Genetics 564, an undergraduate capstone course at UW-Madison.
What is chemical genetics?
|
Have you ever wondered how drugs are discovered, or how they work? Chemical genetics is at the heart of the answer. Drugs are typically small molecules that have the ability to bind to and change the function of a certain protein. The drug can do this because it is able to interact with a certain binding site on it's target protein.
Think of the drug as a hunter, and as the protein as its prey. The hunter enters the system and seeks out its prey. Once the two meet, the hunter interacts with the prey and changes its state of functionality. Drugs can be discovered or created through a process called the small molecule array. |
|
The small molecule array allows for the testing of thousands of different small molecules at once. [1] The process begins by identifying the protein for which you aim to find an interacting drug or small molecule. The protein is tagged with a fluorescent marker. Then, all of the molecules that you want to test are washed over the sites of the proteins. The molecules that interact cause the protein to light up. [1].
Remember, in allergic rhinitis, TGFB1 is the protein we are focusing on. Following the above logic, we would be searching for a drug that directly interacts with TGFB1. However, many drugs act on chemical processes, or signaling pathways, that actually indirectly affect the levels of the target protein by directly interacting with another protein involved in that pathway. The drug and pathway for allergic rhinitis that I will be focusing on is a great example of this.
Remember, in allergic rhinitis, TGFB1 is the protein we are focusing on. Following the above logic, we would be searching for a drug that directly interacts with TGFB1. However, many drugs act on chemical processes, or signaling pathways, that actually indirectly affect the levels of the target protein by directly interacting with another protein involved in that pathway. The drug and pathway for allergic rhinitis that I will be focusing on is a great example of this.
What drug can we use to treat TGFB1 overexpression?

Losartan is an FDA-approved drug to treat high blood pressure. Losartan acts on a specific pathway called the angiotensin ii receptor pathway to decrease the amount of secreted TGFB1. [2] This is an example of a drug that interacts with a protein in a signaling pathway which indirectly leads to the decrease of our target protein, TGFB1. On the right is a small graphic of the pathway which Losartan is involved in. Losartan acts as something called a receptor antagonist. It prevents the angiotensin ii receptor from binding with the molecule that it's supposed to bind with. This decreases the intracellular signaling cascade that usually leads to expression of TGFB1, and therefore decreases the amount of TGFB1 expressed. It remains to be tested whether or not Losartan could relieve allergic rhinitis symptoms by decreasing the amount of TGFB1. [3]
How does Losartan Work?
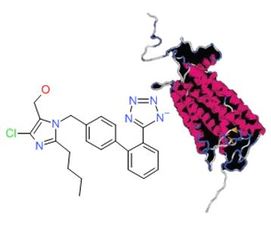
Losartan is a drug that can interact with a protein to alter its function. The protein, angiotensin ii receptor, is shown in the right image, and the chemical structure of Losartan is shown in the left picture. A part of the Losartan molecule acts as the hunter, and targets a specific site of the antiotensin ii receptor protein. This changes the function of the protein to no longer act as the receptor for its intended protein.
Analysis
Losartan is safe for human consumption, and is already used to treat high blood pressure. It acts on the angiotensin ii receptor pathway as a receptor antagonist to block binding of the angiotensin ii receptor and its intended protein, and therefore blocks the secretion of TGFB1. Losartan could have many uses besides high blood pressure. Treating over expression of TGFB1 would be useful to many diseases, including allergic rhinitis.
An additional aspect of Losartan that will be interesting to explore in the future is its known, yet rare, side affect of neutropenia. [4] Neutropenia is the absence or severe reduction of neutrophils in the body's immune system. Neutrophils play an essential role in early allergic rhinitis response, so the possibility that Losartan can actually decrease the amount of neutrophils may be a beneficial factor when it is being used to treat allergic rhinitis.
An additional aspect of Losartan that will be interesting to explore in the future is its known, yet rare, side affect of neutropenia. [4] Neutropenia is the absence or severe reduction of neutrophils in the body's immune system. Neutrophils play an essential role in early allergic rhinitis response, so the possibility that Losartan can actually decrease the amount of neutrophils may be a beneficial factor when it is being used to treat allergic rhinitis.
References
[1] Small molecule microarray. (2017). Scanning Life's Matrix: Genes, Proteins and Small moleules. HHMI Biointeractive. Howard Hughes Medical Institute. http://www.hhmi.org/biointeractive/small-molecule-microarrays
[2] Ripley, E., & Hirsch, A. (2010). Fifteen years of losartan: what have we learned about losartan that can benefit chronic kidney disease patients? International Journal of Nephrology and Renovascular Disease, 3, 93–98.
[3] Frischmeyer-Guerrerio, P. A., Guerrerio, A. L., Oswald, G., Chichester, K., Myers, L., Halushka, M. K., … Dietz, H. C. (2013). TGFβ Receptor Mutations Impose a Strong Predisposition for Human Allergic Disease. Science Translational Medicine, 5(195), 195ra94. http://doi.org/10.1126/scitranslmed.3006448
[4] Das, S., Bandyopadhyay, S., Ramasamy, A., Prabhu, V. V., & Pachiappan, S. (2015). A case of losartan-induced severe hyponatremia. Journal of Pharmacology & Pharmacotherapeutics, 6(4), 219–221. http://doi.org/10.4103/0976-500X.171880
Images/Video
[1] http://www.vmi-group.com/care/
[2] https://www.youtube.com/watch?v=1Ntoml52-K0&t=136s
[3] http://www.jpharmacol.com/article.asp?issn=0976-500X;year=2012;volume=3;issue=1;spage=20;epage=25;aulast=Jananie
[4] https://livertox.nih.gov/Losartan.htm
[2] Ripley, E., & Hirsch, A. (2010). Fifteen years of losartan: what have we learned about losartan that can benefit chronic kidney disease patients? International Journal of Nephrology and Renovascular Disease, 3, 93–98.
[3] Frischmeyer-Guerrerio, P. A., Guerrerio, A. L., Oswald, G., Chichester, K., Myers, L., Halushka, M. K., … Dietz, H. C. (2013). TGFβ Receptor Mutations Impose a Strong Predisposition for Human Allergic Disease. Science Translational Medicine, 5(195), 195ra94. http://doi.org/10.1126/scitranslmed.3006448
[4] Das, S., Bandyopadhyay, S., Ramasamy, A., Prabhu, V. V., & Pachiappan, S. (2015). A case of losartan-induced severe hyponatremia. Journal of Pharmacology & Pharmacotherapeutics, 6(4), 219–221. http://doi.org/10.4103/0976-500X.171880
Images/Video
[1] http://www.vmi-group.com/care/
[2] https://www.youtube.com/watch?v=1Ntoml52-K0&t=136s
[3] http://www.jpharmacol.com/article.asp?issn=0976-500X;year=2012;volume=3;issue=1;spage=20;epage=25;aulast=Jananie
[4] https://livertox.nih.gov/Losartan.htm
